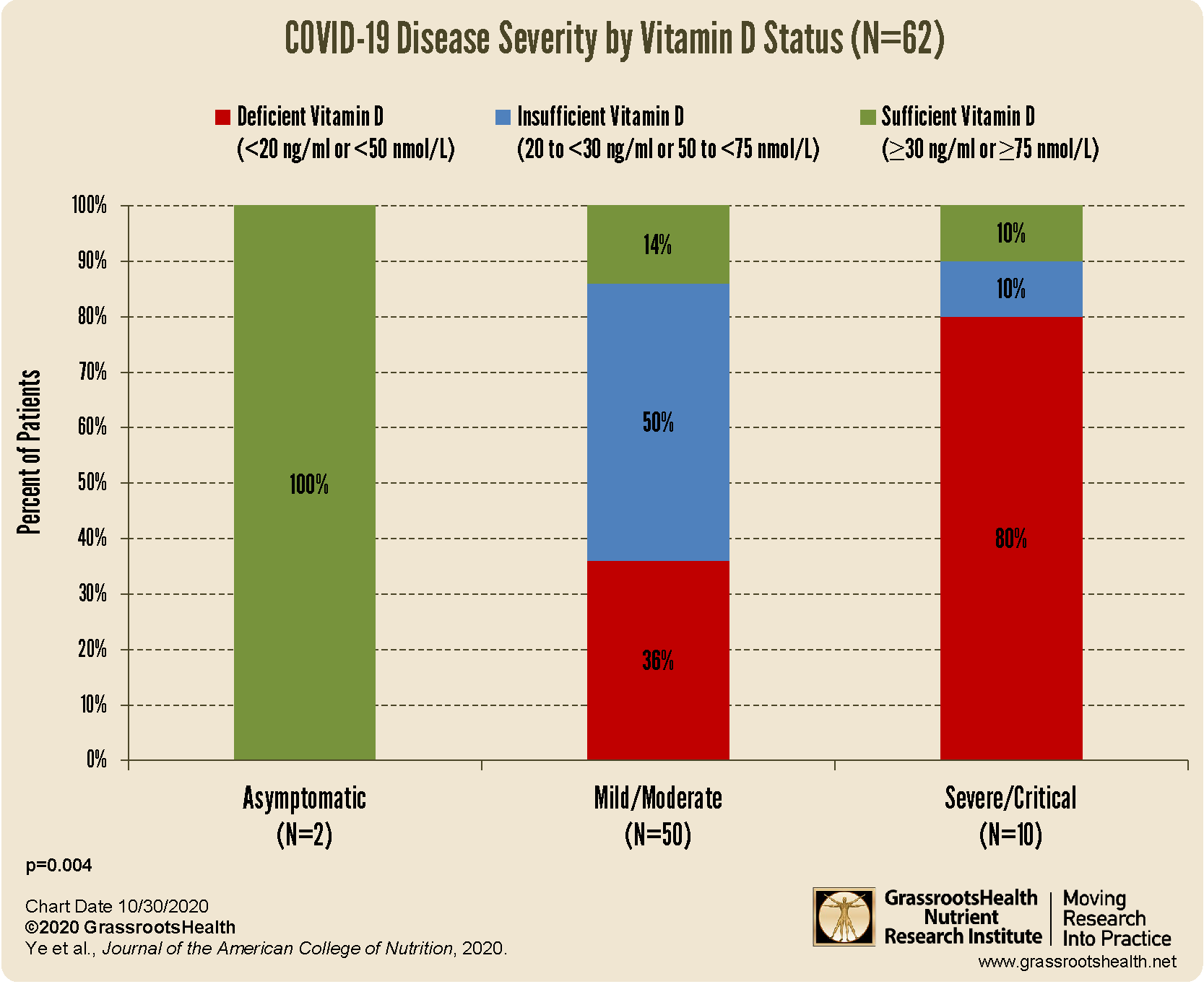
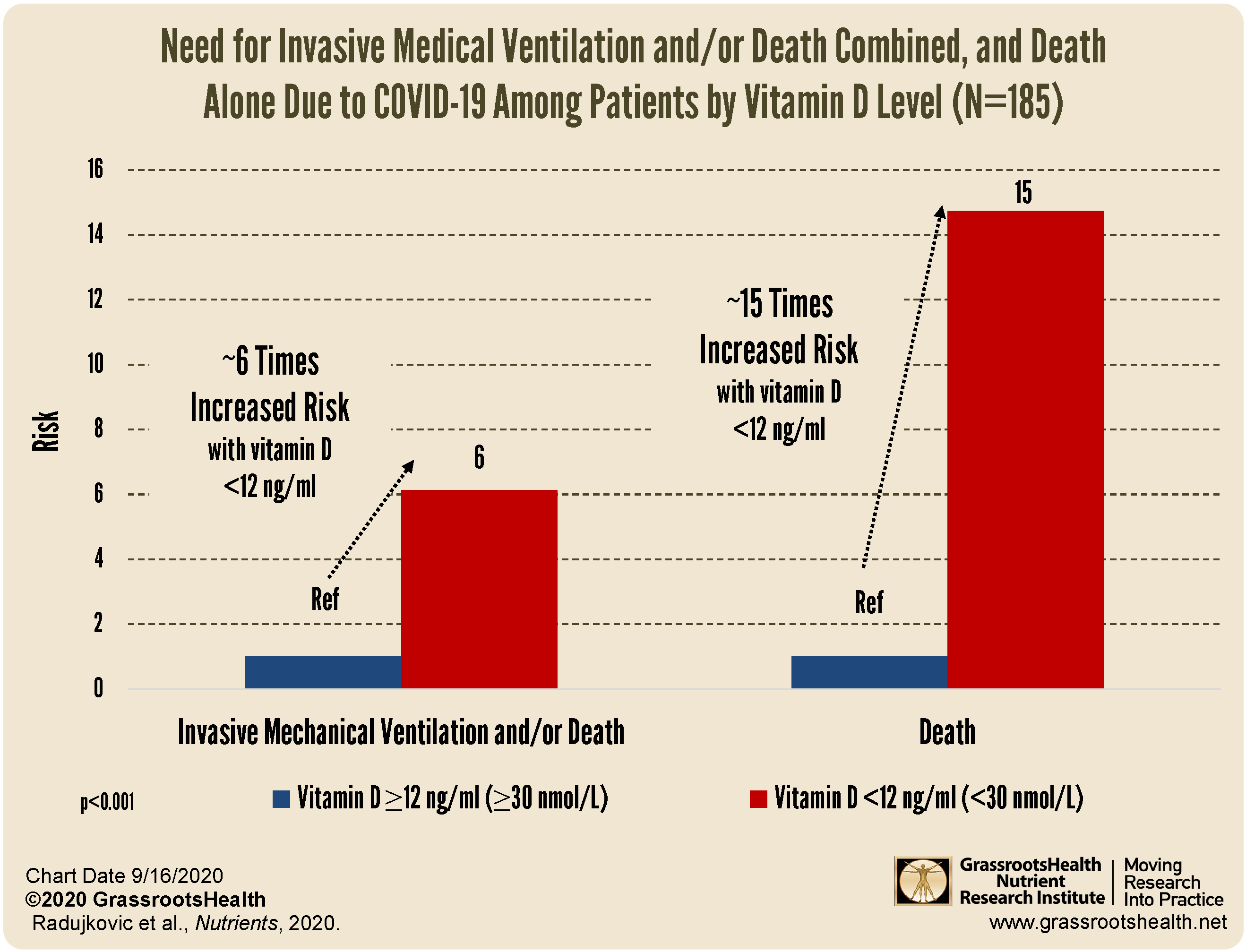
Greek study finds a correlation between vitamin D level and COVID-19 death
 As the new year begins, we will continue to report on the evidence that links vitamin D and COVID-19 disease and severity. Studies have been published concluding that higher vitamin D levels are associated with more positive outcomes, from a decreased risk of testing positive for SARS-CoV-2 to a decreased risk of severity and death. Last week, we shared a study that showed the risk of being hospitalized with COVID-19 is higher with vitamin D deficiency. Below we discuss a study that focuses on patients with COVID-19 that have been admitted to the ICU.
As the new year begins, we will continue to report on the evidence that links vitamin D and COVID-19 disease and severity. Studies have been published concluding that higher vitamin D levels are associated with more positive outcomes, from a decreased risk of testing positive for SARS-CoV-2 to a decreased risk of severity and death. Last week, we shared a study that showed the risk of being hospitalized with COVID-19 is higher with vitamin D deficiency. Below we discuss a study that focuses on patients with COVID-19 that have been admitted to the ICU.
Severity of COVID-19 is associated with inflammatory responses, specifically with the presence of pneumonia, severe acute respiratory distress syndrome, myocarditis (inflammation of the heart muscle), thrombosis (formation of blood clots in the blood vessels) and cytokine storms. We recently reviewed how vitamin D helps prevent inflammation and reduce the severity of COVID-19.
Vitamin D Levels in Patients Admitted to the ICU
In a prospective, observational study, Vassilious and colleagues investigated COVID-19 patients who were admitted to the ICU to see whether low vitamin D levels put them at greater risk of mortality. Critically ill patients diagnosed with COVID-19 pneumonia who were admitted to the ICU of a Greek hospital had their vitamin D levels measured.
Thirty adults, with an average age of 65 years, presented with symptoms of pneumonia 6 days before admission to the ICU, with 90% having acute respiratory distress syndrome (ARDS), mostly moderate or mild. Common risk factors in these patients included hypertension, hyperlipidemia and diabetes. Twenty-three patients required mechanical ventilation and 5 died within 28 days after ICU admission.
80% of Hospitalized COVID-19 Patients Were Vitamin D Deficient, All Were Insufficient
Of the 30 patients admitted to the ICU with COVID-19 pneumonia, 80% (n=24) had vitamin D levels less than 20 ng/ml (50 nmol/L) and classified as deficient, and the remaining 20% (n=6) were considered insufficient with levels between 20 and less than 30 ng/ml (75 nmol/L).
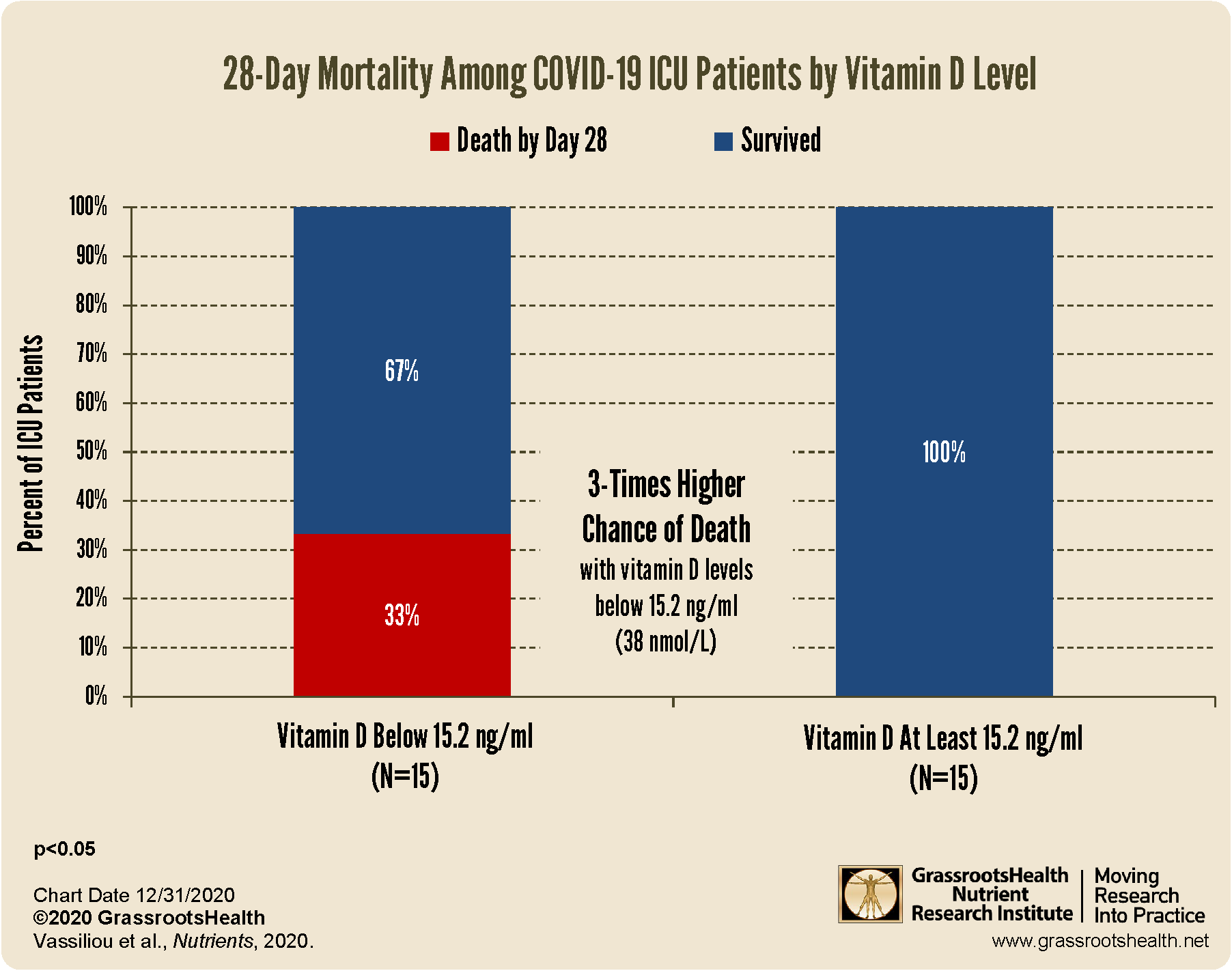
To examine the effect of low vitamin D on mortality, patients were divided as “high” or “low” based on whether they were above or below the median vitamin D level (the middle value) of 15.2 ng/ml (38 nmol/L), a level we would consider to be “severely” deficient. By 28 days, five of the patients with vitamin D levels below 15.2 ng/ml died whereas none of the patients in the group with a vitamin D level of at least 15.2 ng/ml had died.
Risk of Death Higher with Lower Vitamin D Levels
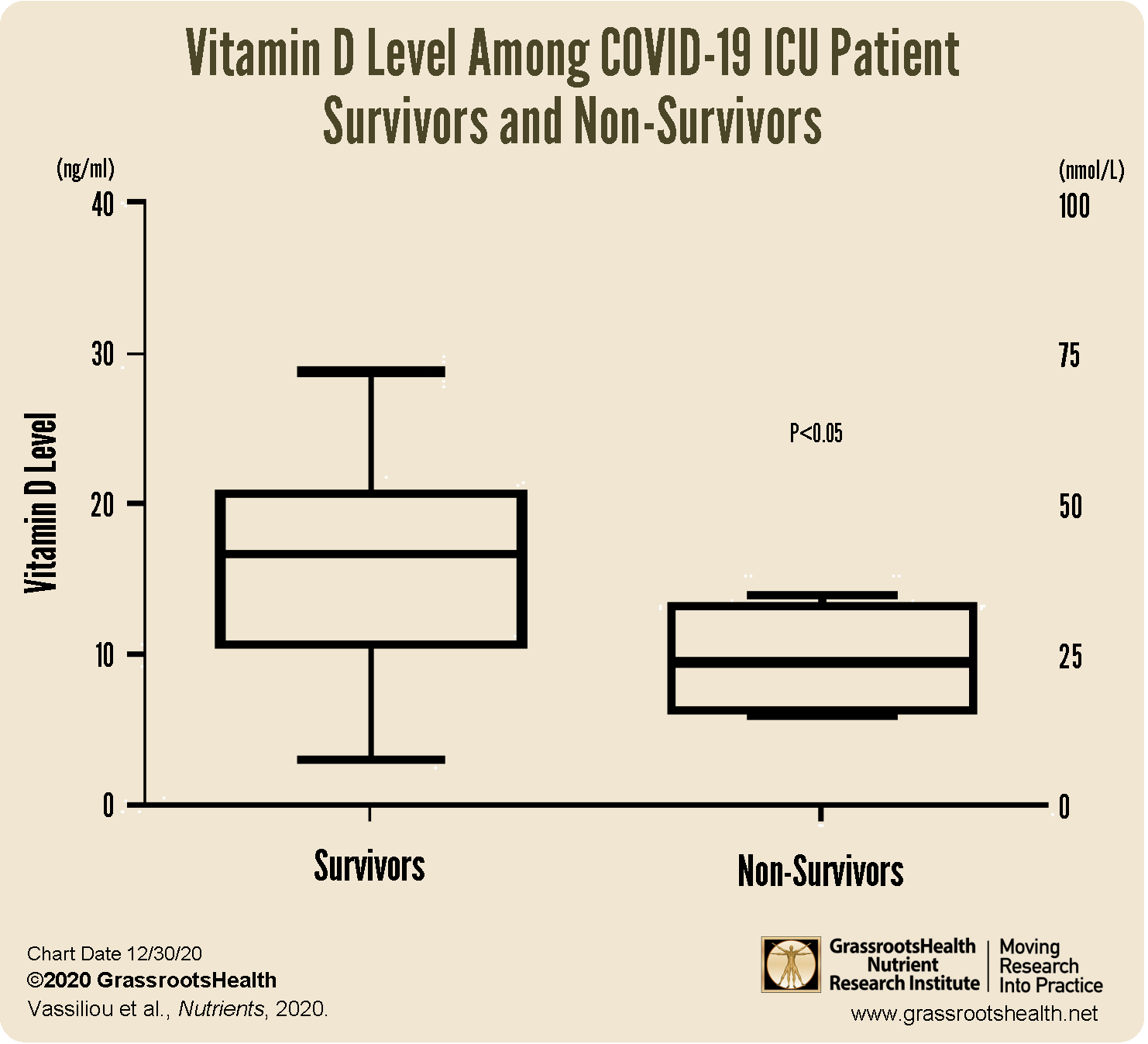
As depicted in the box chart below, vitamin D levels, although insufficient, were higher in patients who survived with a median level of 16.7 ng/ml (42 nmol/L) in comparison with those who died with levels of 9.4 ng/ml (23.5 nmol/L).
All patients belonging to the higher vitamin D group survived, while all non-survivors belonged to the group with lower levels.
Do You Know Your Vitamin D Level?
By joining the GrassrootsHealth projects, you are not only contributing valuable information to our study, but you are also gaining knowledge about how you could improve your own health through measuring and tracking your nutrient status, and educating yourself on how to improve it. Do you know what your status of vitamin D, omega-3s, and other essential nutrients is? Could your levels be improved? Test now to find out!
What does the Research Say about Vitamin D & COVID-19?
It’s TIME to start saving lives! If you can help PREVENT the majority of the death, it’s time! What’s it costing you/us not to take action NOW?
There is much published research that supports a clear link between vitamin D and COVID-19 showing that higher vitamin D levels are related to:
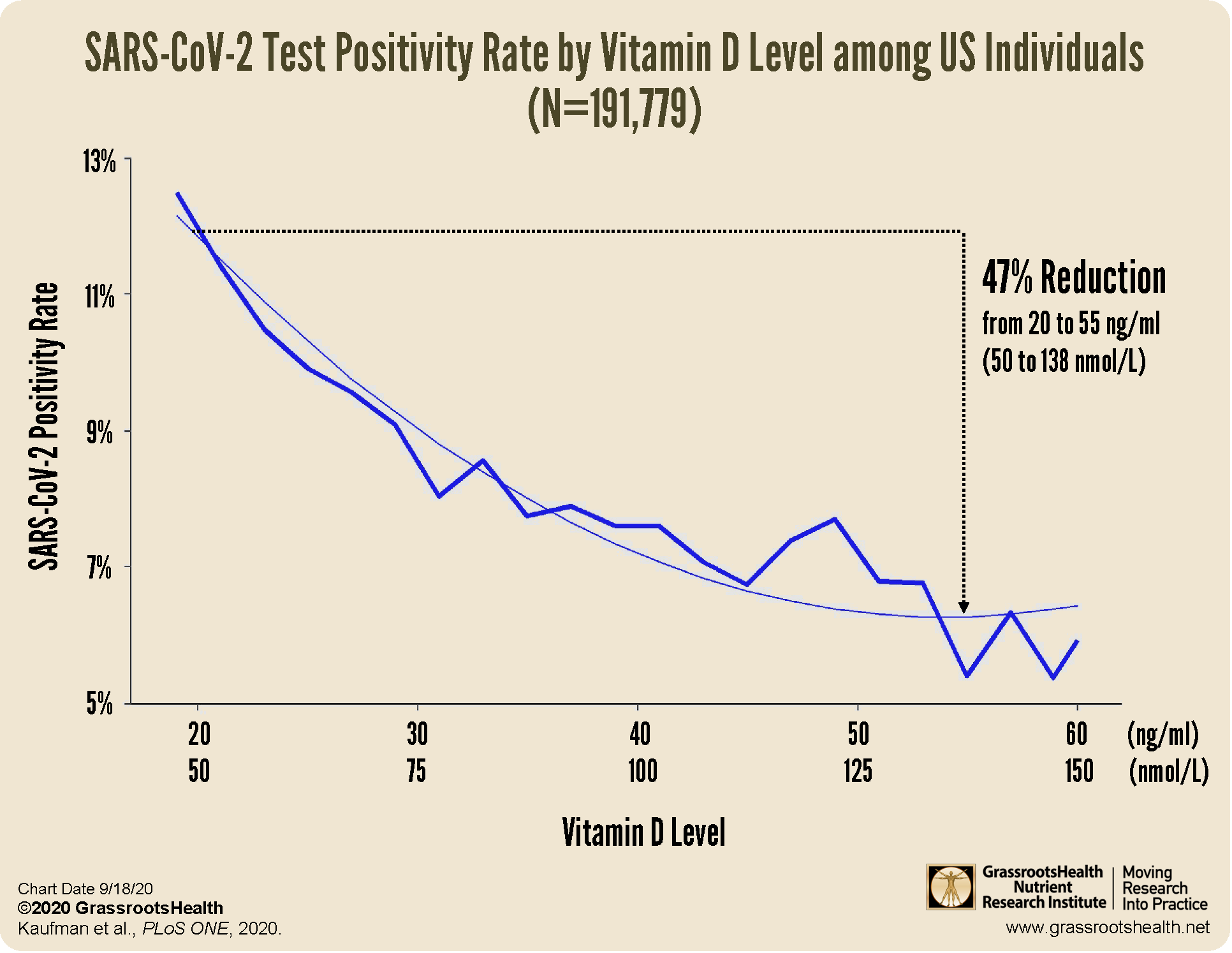
a decreased risk of testing positive for COVID-19
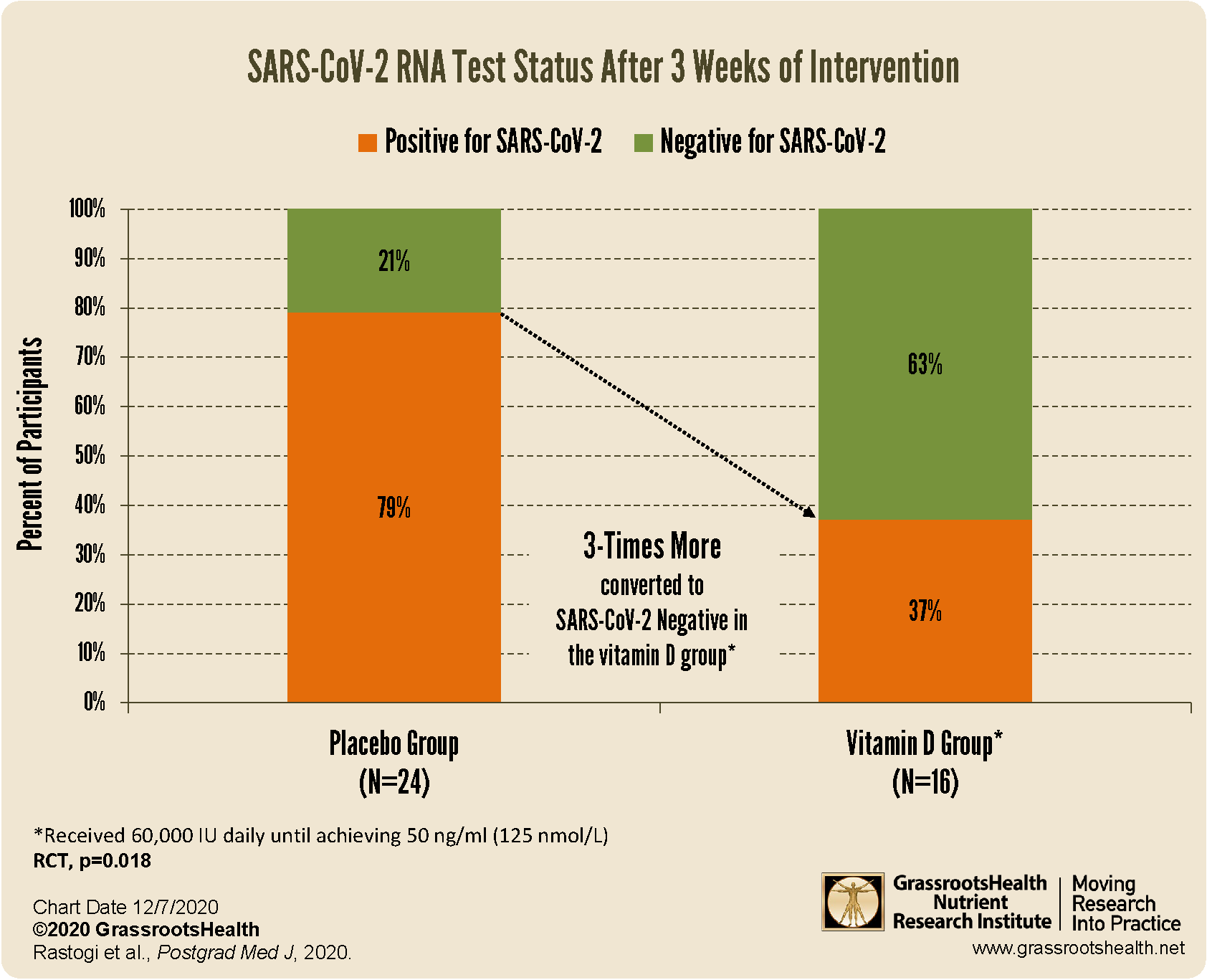 increased viral SARS-CoV-2 RNA clearance
increased viral SARS-CoV-2 RNA clearance
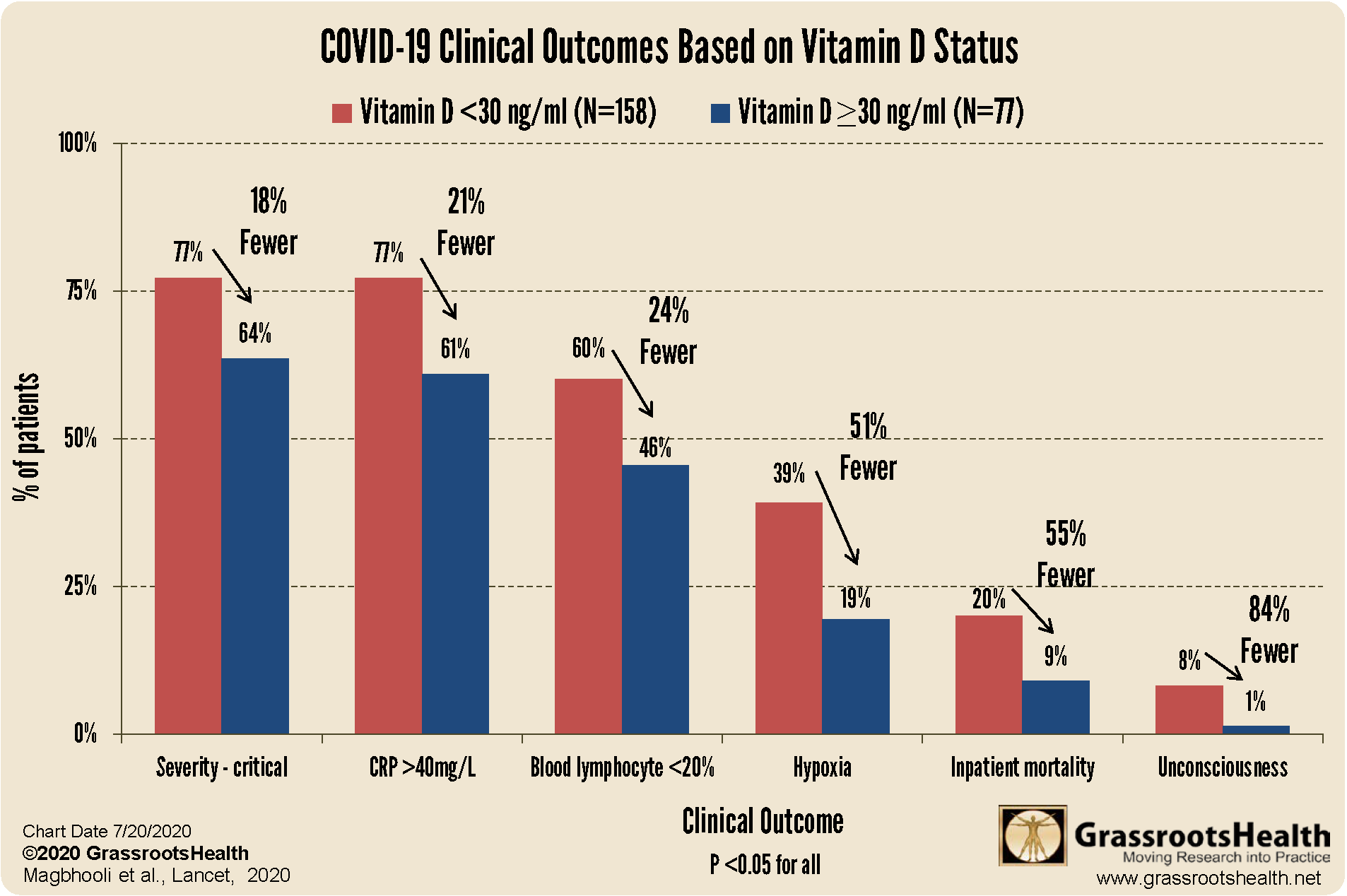
better clinical outcomes among patients with COVID-19
decreased risk of death due to COVID-19
Be sure to educate yourself on the benefits and importance of vitamin D for immune health, and take steps to ensure you and your loved ones are getting enough.
You can review all of the COVID-19 and immune health information we have shared on this page.